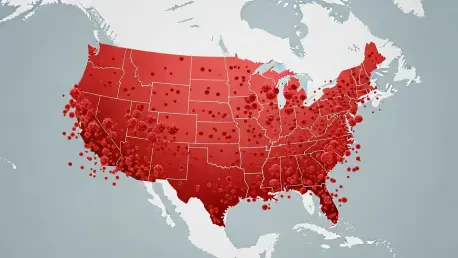
Determining the Scale of Resurgence Through Genomic Surveillance
A sophisticated network of genetic detectives is currently racing to determine if the United States has permanently lost its hard-won status as a nation free from endemic measles transmission. The sudden escalation of measles cases across multiple states has forced federal health officials to confront a reality that seemed unthinkable at the turn of the century. The central question of the current investigation is whether the virus has successfully established a permanent foothold within the borders of the United States, moving silently through communities via continuous transmission chains. If the pathogen has persisted undetected for more than a year, the nation’s official elimination status, a gold standard of public health achievement since the year 2000, will be revoked by international health bodies.
To answer this question, researchers are leaning heavily on genomic surveillance, which acts as a molecular fingerprinting system for the virus. By scrutinizing the genetic architecture of recent cases, scientists can distinguish between a series of unrelated events brought in by international travel and a wider outbreak that is feeding on domestic fuel. This distinction is paramount, as the former represents a manageable challenge, while the latter indicates a fundamental collapse in the national immunity barrier that once protected the most vulnerable members of society. The data gathered from these efforts will provide the definitive evidence required to judge the resilience of the country’s public health infrastructure.
Context of the 2025-2026 Measles Outbreak
The historical achievement of measles elimination in the United States was predicated on a rigorous vaccination infrastructure that ensured over 95 percent of children received the MMR vaccine. According to the criteria established by the World Health Organization, elimination is defined not by the total absence of disease, but by the lack of any chain of transmission that persists for twelve months or longer. Since the year 2000, every domestic outbreak was traced back to an external source, but the sheer volume of cases recorded throughout 2025 and into the first months of 2026 suggests this protective wall has developed significant structural fractures.
The current crisis is unfolding against a backdrop of shifting federal health priorities and a noticeable decline in public trust regarding traditional immunization schedules. As childhood vaccination rates dip below the critical threshold required for herd immunity in various pockets of the country, the risk of a sustained resurgence grows exponentially. This research into the genetic lineage of the virus arrives at a moment when the national public health infrastructure is under unprecedented strain, struggling to balance advanced scientific monitoring with a fractured narrative regarding the necessity of preventative medicine. The outcome of this period will likely redefine national health policy for the coming decade.
Research Methodology, Findings, and Implications
Methodology
The investigative team utilized Whole-Genome Sequencing (WGS), a process facilitated by a partnership between the Centers for Disease Control and Prevention and the Broad Institute. Unlike traditional genotyping, which analyzes only a small portion of the viral genetic material, WGS provides a comprehensive genetic map that captures every mutation across the entire viral genome. This high-resolution approach allows researchers to identify the most subtle changes in the virus as it moves from person to person, essentially creating a forensic timeline of the outbreak’s evolution across different geographic regions.
By tracking these genetic shifts, which typically occur every two to four transmission events, scientists can determine if an outbreak in a state like Texas shares a direct ancestor with a cluster in Utah. This forensic work involves the sequencing of approximately 1,000 inactivated samples, a massive undertaking that requires seamless coordination between federal researchers and state-level laboratories. The methodology relies on the rapid sharing of data to ensure that public health officials can visualize the movement of the virus in near-real-time, rather than relying solely on retrospective epidemiological interviews that are often limited by human memory or incomplete travel records.
Findings
The preliminary data from this genomic investigation has identified the D8-9171 strain as the primary catalyst for the major outbreaks currently observed in Texas, Utah, and South Carolina. This finding is significant because the strain is also highly active in neighboring countries, making it difficult to distinguish between new importations and established domestic spread without the granular detail provided by whole-genome sequencing. The discovery of this dominant strain suggests that the virus is finding fertile ground in unvaccinated clusters, allowing it to hop across state lines with increasing frequency.
Furthermore, the research uncovered significant systemic bottlenecks, specifically a marked delay in data reporting at the federal level compared to the rapid output from localized facilities. While the Utah Public Health Lab demonstrated the capacity for swift genomic analysis, the federal response was hampered by internal staffing shortages and the reallocation of critical funding. These delays have created a gap in the national situational awareness, making it difficult for health officials to implement timely interventions in areas where the virus might be establishing a permanent presence. The lack of a unified speed in data processing has directly impacted the ability to contain the virus before it reaches critical thresholds.
Implications
The most immediate implication of these findings is the high probability that the United States will lose its status as a measles-free nation, a move that would invite intense scrutiny from the Pan American Health Organization and the World Health Organization. Such a downgrade would not merely be a symbolic blow to national prestige; it would likely lead to stricter travel advisories and a requirement for more intensive monitoring protocols. The shift reflects a broader trend where the country is no longer seen as a leader in disease eradication, but rather as a region where preventable illnesses are regaining a foothold due to policy failures.
On a societal level, the research highlights the consequences of a changing federal health discourse that has begun to emphasize alternative health strategies over traditional vaccination. As federal agencies revise their public communication to include more ambiguous language regarding vaccine safety, the resulting confusion among parents has directly contributed to the vaccination gaps being mapped by these genomic studies. This disconnect between state-of-the-art laboratory capabilities and the foundational failure of basic health policy illustrates a paradox where the nation can track the virus with pinpoint accuracy but cannot convince enough of the population to prevent its spread.
Reflection and Future Directions
Reflection
Looking back at the trajectory of this study, there is a profound irony in the fact that millions of dollars and countless hours of high-tech research are being spent to track a disease that was effectively defeated decades ago. The reliance on expensive, cutting-edge technology to monitor a preventable pathogen underscores a regression in public health strategy. While the genomic data provides an objective record of the virus’s movement, it also serves as a stark reminder that technology cannot compensate for the erosion of a once-robust immunization culture. The investigation revealed that the greatest challenge was not the science itself, but the socio-political environment in which the science was conducted.
The researchers involved in this study encountered numerous hurdles, ranging from political interference in the framing of scientific data to the technical challenges of scaling genomic surveillance during an active crisis. If the investigation could be expanded, there would be a significant benefit in integrating real-time socioeconomic data with genetic findings to more accurately predict which communities are most at risk of becoming permanent reservoirs for the virus. This integrated approach would move the focus from merely reacting to outbreaks to proactively identifying and shoring up the specific vulnerabilities that allow the virus to persist in modern society.
Future Directions
Moving forward, it is essential to establish a more transparent and streamlined pipeline for genomic data sharing that is insulated from political fluctuations and administrative delays. The success of state labs during this period provides a model for a decentralized surveillance network that can respond to local surges without waiting for federal approval. Developing these pathways now will be critical for managing future outbreaks of other vaccine-preventable diseases that may follow in the wake of the current measles resurgence. The resilience of the national health system depends on the ability to turn laboratory data into actionable community health interventions.
Additionally, future research should investigate the long-term impact of federal policy shifts on childhood immunization rates across diverse demographics to understand how to best rebuild public trust. There is also potential for the whole-genome sequencing protocols developed during this crisis to become a new global standard for epidemiological analysis in other nations approaching elimination. By refining these tools, the international community can create a more resilient defense against the resurgence of infectious diseases, ensuring that the hard-won gains of the past century are not permanently lost to a rising tide of misinformation and policy neglect.
Assessment of National Health Strategy and Elimination Status
The final evaluation of the national health strategy reveals that while genomic science has provided an unparalleled view of the virus’s path, it remains an insufficient substitute for the preventative power of high vaccination coverage. The verdict on the nation’s elimination status ultimately reflected whether the current trajectory prioritized individual health choices over the collective security of the population. This period of resurgence demonstrated that the infrastructure designed to protect public health was more fragile than previously assumed, particularly when scientific consensus was weighed against ideological shifts. The reliance on retrospective genomic data showed that the virus had already established a presence before the state could effectively respond.
The findings from the genetic mapping project confirmed that the tools to stop the spread were always available, yet the application of those tools was compromised by a lack of consistent, evidence-based policy. It was concluded that a successful national health strategy must align innovation with a commitment to the foundational principles of immunization to maintain long-term health security. Ultimately, the lessons learned from this challenge provided a clear indication that safeguarding a nation’s health requires more than just advanced data; it demands a unified social contract toward the protection of the entire community through proven medical practices. This investigation proved that once elimination is lost, the road to recovery is far more costly than the efforts required to maintain it.