The long-standing struggle to manage chronic high blood pressure has finally encountered a formidable adversary that does not rely on a patient’s ability to remember a daily pill. For decades, the medical community has battled the “silent killer” using a standard arsenal of pharmaceuticals, yet millions of individuals continue to live under the constant shadow of potential strokes and heart attacks. This stagnation stems from a combination of physiological resistance and the practical reality of medication non-compliance. However, a transformative shift is occurring as renal denervation (RDN) moves from a clinical theory toward a primary tool in the cardiovascular toolkit. By offering a biological “reset” for the sympathetic nervous system, this procedure provides a persistent defense that functions independently of human error or digestive variability.
The End of the “Silent Killer” Stalemate
Traditional hypertension management often feels like a perpetual game of catch-up, where physicians adjust dosages and switch prescriptions while blood pressure remains stubbornly high. The physiological complexity of the human body means that many patients eventually hit a wall where additional medications yield diminishing returns or intolerable side effects. This cycle of “pill fatigue” contributes to a dangerous environment where hypertension remains uncontrolled in a significant portion of the global population. The emergence of renal denervation represents a fundamental departure from this reactive pharmaceutical model, introducing a localized intervention designed to quiet the overactive signals that drive chronic elevation.
By shifting the focus from temporary chemical suppression to a physical modification of the renal nerves, medical professionals are discovering a more reliable path to stability. This “always-on” approach addresses the root cause of the “fight or flight” response that often malfunctions in hypertensive individuals. Unlike tablets that peak and fade throughout the day, the procedural intervention aims to lower the baseline pressure permanently. This shift is particularly critical for high-risk patients who have spent years cycling through various drug classes without achieving their target goals, finally offering a way to break the stalemate against cardiovascular decay.
Understanding the Shift in Cardiovascular Intervention
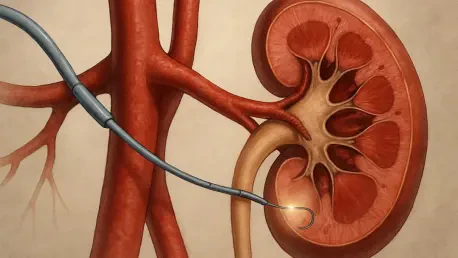
The landscape of cardiovascular care is currently moving away from general systemic treatments toward targeted procedural interventions that address specific biological triggers. Renal denervation, particularly through advanced radiofrequency systems like Medtronic’s Symplicity Spyral, focuses on deactivating hyperactive sympathetic nerves located within the walls of the renal arteries. This technique utilizes a catheter-based delivery system to apply precise energy, effectively dampening the signals between the brain and the kidneys. The recent clearance of these technologies by regulatory bodies marks a transition from experimental research to a standard of care for those who are most vulnerable to the consequences of uncontrolled hypertension.
This evolution signifies a broader trend in modern medicine where the goal is to reduce the total burden of chronic disease management for the patient. While lifestyle changes and medication will likely always play a role, the inclusion of a one-time procedure allows for a more proactive preventative strategy. By targeting the nervous system’s role in blood pressure regulation, clinicians can provide a stabilizing force that remains effective regardless of external factors. As the technology matures, it is becoming clear that the future of hypertension care lies in this synergy between traditional therapy and advanced biological interventions.
The Evolution of Clinical Evidence and Strategic Application
Rigorous clinical evaluation is currently expanding the scope of how renal denervation is applied, specifically within complex medical scenarios that involve multiple cardiovascular risks. A primary example is the EMBRACE trial, which investigates the efficacy of performing RDN simultaneously with coronary stenting for patients with multivessel disease. This integrated strategy aims to reduce residual cardiovascular risk by addressing both the physical blockage in the heart and the underlying systemic pressure at the same time. By consolidating these procedures, the medical system can provide a comprehensive solution in a single intervention, potentially improving long-term outcomes for the highest-risk demographics.
Longitudinal data also supports the durability of this approach, with three-year findings from major clinical programs showing a sustained reduction in hypertensive events. The evidence suggests that patients who undergo the procedure experience significantly fewer blood pressure “spikes” that typically lead to emergency room visits. Furthermore, the economic argument for widespread adoption is becoming harder to ignore. With the potential to save the healthcare system hundreds of millions of dollars by preventing heart failure hospitalizations and acute crises, the transition toward RDN is supported by both clinical success and fiscal responsibility within modern value-based care frameworks.
Expert Perspectives on the Treatment Gap
Prominent figures in the field of cardiology argue that the “treatment gap” between pharmaceutical intervention and target blood pressure levels is one of the greatest hurdles in public health. Experts like Dr. Roxana Mehran have noted that for many individuals, the standard of care simply is not enough to mitigate the risks of long-term organ damage. Clinical data confirms that renal denervation not only lowers pressure but also allows for a substantial reduction in the overall number of medications a patient must take. This improvement in quality of life is a major driver of the technology’s adoption, as it removes the psychological and physical burden of complex daily regimens.
Industry leadership views this transition as a pivotal moment for value-based healthcare, where the focus is on long-term stability rather than short-term symptom management. By providing a procedure that offers years of protection, the medical community is moving toward a model that prioritizes patient outcomes over the continuous cycle of prescription refills. This perspective shifts the narrative of hypertension from a condition that must be constantly managed to one that can be structurally addressed. As more practitioners witness the long-term benefits in their own clinics, the consensus is building that RDN is an essential component of the modern cardiovascular strategy.
Integrating Renal Denervation into Modern Practice
Successful implementation of this technology requires a strategic framework that prioritizes the identification of the most suitable candidates. Healthcare providers are now focusing on patients who remain hypertensive despite intensive drug therapy or those who suffer from severe adverse reactions to common antihypertensive medications. By utilizing a “one-stop shop” model, where RDN is paired with other necessary cardiovascular procedures, hospitals can maximize the impact of every patient encounter. This coordinated approach not only improves the patient experience but also optimizes the use of specialized medical resources and surgical facilities.
To ensure the long-term success of these interventions, clinics are adopting advanced monitoring protocols that emphasize 24-hour ambulatory blood pressure tracking. This allows physicians to verify the ongoing efficacy of the procedure and make precise adjustments to any remaining medication requirements. Navigating the reimbursement landscape has also become more streamlined as insurance providers recognize the cost-benefit of avoiding acute cardiovascular events. The future of hypertension care was built upon the integration of these procedural solutions, ensuring that the most effective tools were available to those who needed them most. Healthcare systems prioritized the development of specialized centers that combined diagnostic precision with the therapeutic power of renal denervation to redefine the standard of care for millions.