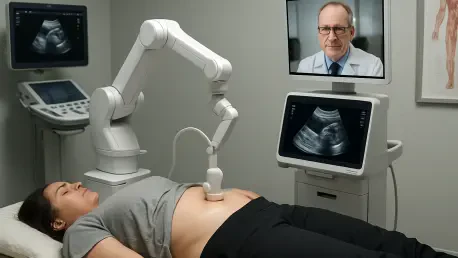
The ability to perform a life-saving medical procedure from a continent away has finally moved from the realm of speculative fiction into a tangible clinical reality for the global medical community. The geographic isolation of extreme environments often means that specialized medical diagnostics remain out of reach for those who need them most. Whether it is a researcher in the frozen wilderness of Antarctica or a resident in a remote mountain village, the physical absence of a trained sonographer can turn a manageable condition into a life-threatening crisis. Tele-robotic ultrasonography (TUS) addresses this disparity by enabling real-time clinical examinations through a sophisticated blend of robotics and high-speed communication.
This technological integration removes the necessity for a specialist to be in the same room, or even the same hemisphere, as the patient. By leveraging artificial intelligence to assist in probe placement and data interpretation, the system creates a bridge between urban centers of excellence and the world’s most inaccessible locations. The core question shifts from whether a patient can reach a doctor to how quickly a robotic interface can bring the doctor’s expertise to the patient’s bedside.
Bridging Global Distances through Tele-Robotic Innovation
The core challenge of modern diagnostics lies in the uneven distribution of specialized human capital across the globe. While urban hospitals are often saturated with experts, rural clinics struggle to provide even basic imaging services. Tele-robotic innovation seeks to solve this by creating a virtual presence for the specialist. Through a remote-controlled interface, a radiologist can manipulate an ultrasound probe with the same precision they would exercise in person, effectively neutralizing the disadvantage of distance.
This solution is particularly vital for real-time examinations where static images or pre-recorded videos are insufficient. In cases of internal bleeding or cardiac distress, the diagnostic process must be dynamic and responsive to the patient’s immediate condition. Robotics and artificial intelligence work in tandem here to ensure that the remote specialist receives high-fidelity data while the robot maintains the necessary physical contact with the patient.
The Evolution of Remote Diagnostics in Extreme Environments
A landmark demonstration recently showcased this potential by linking the All India Institute of Medical Sciences (AIIMS) in New Delhi with the Maitri Research Station in Antarctica. This 12,000-kilometer live trial represents a pivotal moment in the history of tele-medicine, proving that even the most hostile environments can be integrated into a national healthcare network. The success of this connection highlights a significant leap in polar research capabilities, where medical autonomy is often limited by seasonal travel restrictions.
Beyond its scientific novelty, this breakthrough addresses the critical global shortage of specialized sonographers in rural and underserved areas. By demonstrating that a radiologist in a capital city can operate a probe at the bottom of the world, the project validates a model for medical sovereignty. This approach allows nations to provide a high standard of care to their citizens regardless of their location, effectively democratizing access to advanced diagnostic tools that were previously reserved for elite urban hospitals.
Research Methodology, Findings, and Implications
Methodology
The development of the TUS system relied on a robust collaborative framework involving premier engineering institutions, medical experts, and polar research organizations. The technical architecture features a robotic arm with six degrees of freedom, designed to replicate the complex rotational and translational movements of a human hand. Integrated force-sensing capabilities were essential to this design, providing the system with the “touch” required to press a probe against a patient’s body with the appropriate pressure without causing discomfort or injury.
To maintain a seamless connection over such a vast distance, the team utilized a dedicated communication infrastructure optimized for low-latency data transmission. This setup ensured that the visual feedback from the ultrasound machine and the haptic commands from the operator remained synchronized. By utilizing satellite links and advanced data compression algorithms, the researchers successfully mitigated the lag that typically plagues long-distance remote operations.
Findings
The trial between Delhi and Antarctica produced high-resolution images of abdominal organs and cardiac structures, matching the quality of scans performed in person. A key finding was the achievement of sub-second latency, a threshold that allowed the radiologist to adjust the probe position in real-time based on the live video feed. This responsiveness proved critical during simulated trauma scenarios, where the system successfully performed Focused Assessment with Sonography for Trauma (FAST) scans.
These results confirm that the robotic interface is sensitive enough to detect subtle pathological changes even when the operator is thousands of miles away. The ability to conduct emergency screenings remotely suggests that the technology is ready for more than just routine check-ups. It demonstrated a high level of reliability under the fluctuating bandwidth conditions typical of polar regions, reinforcing the system’s viability for real-world deployment in unpredictable environments.
Implications
The deployment of TUS technology fundamentally optimizes healthcare logistics by providing a reliable method for remote triage. In environments like Antarctica or deep-sea vessels, the cost and risk associated with emergency medical evacuations are immense; however, a quick robotic scan can determine if an evacuation is truly necessary. This capability preserves resources and ensures that high-risk transport is reserved for patients who cannot be managed on-site.
On a broader societal level, the availability of affordable and portable robotic units could revolutionize rural healthcare. Disaster zones and conflict regions, where medical infrastructure is often destroyed or non-existent, stand to benefit from the rapid deployment of these systems. Furthermore, the integration of AI-assisted guidance helps standardize diagnostic quality, ensuring that a patient in a village receives the same level of care as one in a metropolitan center.
Reflection and Future Directions
Reflection
Achieving this level of technical synergy required a comprehensive “whole-of-government” approach, merging the distinct priorities of engineering, clinical practice, and logistical management. The project served as a testbed for interdisciplinary cooperation, revealing the complexities of translating laboratory robotics into a bedside medical tool. One of the primary technical challenges involved ensuring patient safety through haptic feedback loops that could compensate for signal jitters across continents.
The evaluation of the current prototype indicates a high degree of readiness for mass-market adoption, though scalability remains a focus for further refinement. While the initial costs of developing such specialized equipment are significant, the potential for mass production could lower the barrier to entry for smaller clinics. The success of the Delhi-Antarctica link has provided the necessary confidence to move from a proof-of-concept phase toward a broader clinical implementation strategy.
Future Directions
Moving forward, the focus will shift toward developing fully autonomous AI-driven scanning protocols that can assist non-specialist operators in the field. Such systems could potentially guide a local health worker through the steps of a complex scan, with the robot taking over the fine-tuning of the probe position. This evolution would further reduce the burden on specialists and allow for more frequent monitoring of chronic conditions in remote populations.
Research is also expanding into the use of tele-robotics for even more extreme frontiers, including deep-sea exploration and future long-duration space missions. Investigating the long-term economic benefits will be essential for integrating these systems into national public health infrastructures. By reducing the reliance on physical proximity, the medical community can move toward a future where diagnostic expertise is treated as a ubiquitous digital utility rather than a localized physical service.
A New Paradigm for Universal Healthcare Access
The successful implementation of tele-robotic ultrasound fundamentally redefined the possibilities of modern clinical workflows. This breakthrough proved that specialized remote care was not only feasible but also sustainable for the most vulnerable populations on the planet. By validating the link between Delhi and the Antarctic coast, the research established a template for how integrated science could overcome the physical barriers that had long hindered global health equity.
The project demonstrated that technological independence was a key driver of medical progress, allowing nations to build resilient systems tailored to their specific geographic challenges. In the coming years, the refinement of these robotic interfaces will likely lead to a more inclusive healthcare landscape where distance is no longer a factor in the quality of care received. Governments and health organizations must now prioritize the deployment of these portable units to ensure that universal health access becomes a practical reality rather than just a policy goal.