James Maitland is a seasoned expert in the intersection of medical robotics and IoT applications, bringing years of experience in navigating the complex regulatory landscapes that govern patient safety. In this discussion, we explore the critical failures in manufacturing and quality control that led to a significant FDA intervention in the cardiovascular device sector. The conversation delves into the systemic breakdowns in risk assessment, the vital importance of sterile manufacturing environments, and the serious clinical consequences of equipment failure during high-stakes heart procedures.
When syringes used in cardiovascular procedures disconnect from manifolds due to manufacturing issues like excess silicone, what immediate clinical risks arise for the patient, and how should medical teams manage the sudden potential for a life-threatening air embolism?
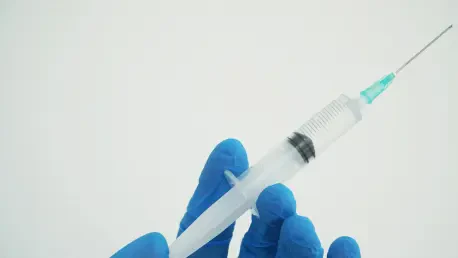
The immediate danger when a syringe disconnects during a delicate cardiovascular procedure is the rapid introduction of atmospheric air into the patient’s vascular system. Because these specific NAMIC syringes are designed to inject contrast dye directly into blood vessels, any structural failure at the connector—often caused by lubricating agents like excess silicone—creates a vacuum that pulls air into the bloodstream. This can result in a fatal air embolism, a condition the manufacturer’s own internal analysis identified as the most severe possible failure mode. Medical teams must maintain a state of hyper-vigilance, immediately stopping the injection the moment a manifold breach is suspected to prevent air from traveling to the heart or brain. Beyond the immediate physical risk, these disconnections often lead to biohazard exposure for clinicians, necessitating a dual-response protocol to protect both the patient on the table and the medical staff in the room.
If a manufacturing facility sees hundreds of safety reports involving biohazard exposure or device failure, how should they re-evaluate their internal risk analysis, and what specific steps are necessary to ensure their safety ratings align with actual clinical outcomes?
When a company receives 221 complaints and is forced to file 177 safety reports, it is a clear indicator that their internal risk metrics are fundamentally broken. In this instance, the facility’s decision to rate the overall risk as “low” despite identifying air embolism as a critical failure was a massive oversight that the FDA found completely inconsistent with reality. To fix this, a manufacturer must move away from subjective “low-risk” labeling and adopt a quantitative approach where clinical failures, such as a patient suffering an embolism, automatically trigger a high-severity rating. This re-evaluation must include a transparent audit of why the data from the 177 safety reports did not lead to immediate corrective actions earlier in the process. True alignment with clinical outcomes requires the engineering team to step out of the lab and analyze how their syringes are performing in the high-pressure environment of a cardiac catheterization suite.
When initial corrective actions fail to lower defect rates and complaints continue to breach safety limits every quarter, what specific changes to manufacturing processes and design testing are required to prevent a full product recall or federal seizure?
If complaint rates are rising throughout an entire year and breaching safety limits every single quarter, as seen throughout 2025, it proves that the initial “band-aid” fixes were wholly inadequate. At this stage, the manufacturer must halt production and perform a deep-dive root cause analysis into the design modifications that allowed excess silicone to compromise the manifold connection. Preventing a federal seizure or court action requires a complete overhaul of the quality management system, shifting from reactive troubleshooting to proactive design validation. This might involve redesigning the connector geometry or implementing automated vision systems on the assembly line to detect silicone levels with micron-level precision. Ultimately, if the company cannot prove that the hardware is safe, they must follow the path of the March 2026 recall and remove the product from the market entirely before regulators take more punitive legal actions.
Given that poor cleaning practices and insufficient testing after design modifications can trigger regulatory warnings, what rigorous protocols should be implemented to maintain sterile environments and ensure that every hardware update meets the highest safety standards?
Maintaining a sterile manufacturing environment requires more than just standard operating procedures; it demands a culture of absolute compliance where cleaning protocols are audited with the same intensity as the final product. When a facility is cited for poor cleaning, it suggests a systemic breakdown in the hygiene barriers that prevent contamination of devices used in the human bloodstream. To ensure hardware updates are safe, companies must implement “worst-case” testing protocols after every design change, simulating the most extreme pressures and temperatures the syringe will face during a heart procedure. This means that if a connector is modified, it must undergo hundreds of cycles of manifold attachment and detachment to ensure that variables like silicone migration do not occur. Rigorous testing must also include biohazard containment drills to ensure that no hardware failure could ever result in a clinician being exposed to a patient’s bodily fluids.
What is your forecast for medical device quality control and regulatory enforcement in the cardiovascular equipment sector?
I anticipate that the FDA will become significantly more aggressive in its enforcement, moving away from simple warning letters toward faster financial penalties and product seizures for repeat offenders. We are entering an era where data transparency will be mandatory; regulators will likely demand real-time access to a company’s complaint logs if they show a trend of breaching safety limits for more than two consecutive quarters. In the cardiovascular sector specifically, the margin for error is effectively zero, so we will see a shift toward “smart” manufacturing where IoT sensors track every drop of lubricant and every sterile seal in real-time. Companies that continue to ignore the warning signs of rising defect rates, as we saw in the NAMIC division case, will find themselves unable to operate in the U.S. market as the gap between manufacturing data and clinical reality finally closes.