I’m thrilled to sit down with James Maitland, a renowned expert in robotics and IoT applications in medicine, whose passion for integrating technology into healthcare has revolutionized patient care solutions. Today, we’re diving into the groundbreaking American Heart Association Connected Care pilot program in collaboration with Cadence, a leader in remote chronic disease monitoring. Our conversation explores how this initiative is transforming post-discharge care for heart failure patients, the innovative technology behind it, the challenges of reducing hospital readmissions, and the broader impact on healthcare costs and patient outcomes. Join us as we uncover the potential of remote monitoring to reshape the future of heart failure management.
How did you first become involved in exploring technology solutions like remote monitoring for heart failure care, and what excites you most about this field?
My journey started with a fascination for how robotics and IoT could solve real-world problems in healthcare. Early in my career, I saw firsthand how patients, especially those with chronic conditions like heart failure, struggled after leaving the hospital. The idea of using connected devices to bridge that gap between hospital and home care was incredibly compelling. What excites me most now is seeing programs like the American Heart Association Connected Care pilot come to life—combining cutting-edge tech with clinical expertise to keep patients healthier and out of the hospital. It’s about giving people their lives back through innovation.
Can you walk us through the main goals of the American Heart Association Connected Care pilot program and how it aims to transform post-discharge care?
The primary goal of this pilot is to tackle the high rate of 30-day readmissions for heart failure patients, which affects nearly one in four individuals after discharge. It focuses on filling critical gaps in care by integrating remote monitoring into the transition from hospital to home. The program aims to provide proactive, timely support through technology, ensuring patients stick to guideline-directed therapies and receive immediate clinical attention when needed. Ultimately, it’s about extending the quality of hospital care into patients’ homes and preventing avoidable readmissions.
What role does the partnership between the American Heart Association and Cadence play in making this program effective?
This collaboration is a powerful blend of expertise and innovation. The American Heart Association brings its gold-standard scientific guidelines and deep understanding of heart failure management, while Cadence offers advanced remote monitoring technology and an always-on virtual care team. Together, they create a seamless system where patients get personalized, evidence-based support anytime, anywhere. It’s a synergy that ensures both the clinical and technological aspects of care are optimized for the best outcomes.
How does the program actually work for patients once they’re discharged from the hospital?
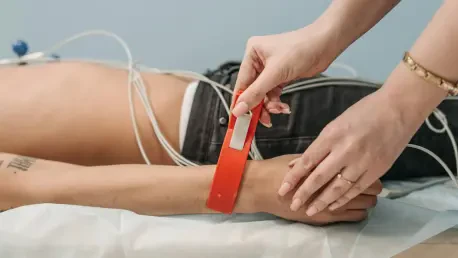
Once patients leave the hospital, they’re enrolled in the program and provided with connected vital sign monitors. They’re taught how to use these devices to track key health metrics like blood pressure or weight, which are critical for heart failure management. A virtual care team from Cadence monitors this data in real-time, offering ongoing clinical support, adjusting treatments as needed, or directing patients to in-person care if there’s an urgent issue. It’s like having a healthcare team in your pocket, ensuring no one falls through the cracks.
What can you tell us about the hospitals involved in this pilot and why they were selected for this initiative?
The pilot includes four hospitals across different regions, each with unique strengths in community care. These facilities were chosen for their commitment to improving patient outcomes and their ability to integrate this program into their discharge workflows. Their diverse settings also help test the scalability of the model across various healthcare environments, ensuring the insights gained can benefit a wide range of hospitals and patient populations in the future.
Why do you think the readmission rate for heart failure patients is so high, and what are the biggest hurdles they face after leaving the hospital?
The high readmission rate—about 25% within 30 days—stems from several challenges. Many patients struggle with adhering to complex medication regimens or recognizing early warning signs of worsening conditions. There’s often a lack of consistent follow-up care, and social factors like limited access to resources or support systems play a big role. After discharge, patients can feel overwhelmed or isolated, and without proper monitoring, small issues can quickly escalate into emergencies requiring rehospitalization.
How does this pilot program address those specific challenges to help keep patients out of the hospital?
The program directly tackles these issues by providing continuous monitoring and support. With connected devices, patients’ health data is tracked in real-time, so the virtual care team can spot potential problems early and intervene before they become serious. It also focuses on education and empowerment, helping patients understand their treatment plans and stick to them. By maintaining that close connection post-discharge, the program reduces the sense of isolation and ensures patients have access to care when they need it most.
There’s been a significant improvement in guideline-directed medical therapy uptake through this kind of remote monitoring. Can you explain how that’s achieved?
Absolutely, the jump from 7% to 23% uptake in guideline-directed therapy is remarkable. It’s largely due to the personalized support patients receive through the virtual care team. They provide ongoing education about the importance of these therapies, reminders to take medications, and adjustments to treatment plans based on real-time data. This consistent engagement builds trust and helps patients overcome barriers like misunderstanding their condition or fear of side effects, leading to better adherence and improved health.
The program also reports substantial cost savings, averaging over $1,000 per patient each month. Can you break down where those savings come from and how they impact the healthcare system?
These savings primarily come from reducing hospital readmissions and emergency visits, which are incredibly costly for both patients and healthcare systems. By catching issues early through remote monitoring, the program prevents expensive acute care episodes. Additionally, optimizing treatments and improving adherence reduces the need for more intensive interventions down the line. For patients, this means lower out-of-pocket costs, and for hospitals, it frees up resources to focus on other critical areas, creating a win-win situation.
Looking ahead, what is your forecast for the role of remote patient monitoring in the future of heart failure management and healthcare as a whole?
I’m incredibly optimistic about the trajectory of remote patient monitoring. As technology continues to advance, I see it becoming a cornerstone of chronic disease management, not just for heart failure but across a range of conditions. We’re moving toward a future where healthcare is more proactive and personalized, with AI and IoT enabling real-time insights and interventions. Programs like this pilot are just the beginning—they’ll pave the way for broader adoption, especially in underserved areas, ultimately making high-quality care accessible to everyone, everywhere.