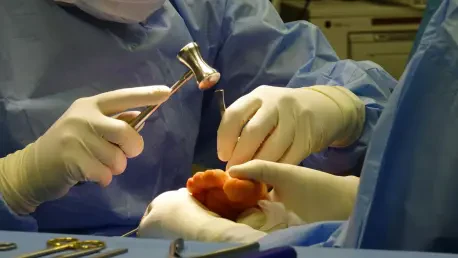
The announcement of a mandatory national expansion for orthopedic care signals a fundamental shift in how the federal government approaches the economics of surgical recovery and patient rehabilitation. By introducing the CJR-X model, the Centers for Medicare & Medicaid Services (CMS) is establishing the first nationwide mandatory episode-based payment system within original Medicare, specifically targeting hip, knee, and ankle replacements. This initiative is designed to replace fragmented, fee-for-service interactions with a cohesive strategy that forces hospitals to oversee the entire patient journey from the initial surgery through ninety days of post-operative care. This policy shift reflects an urgent need to stabilize healthcare expenditures while ensuring that the quality of life for seniors undergoing major joint procedures remains a top priority. As the healthcare landscape transitions toward this new standard, the integration of hospital services with post-acute settings will become the primary benchmark for institutional success, effectively ending the era of isolated clinical interventions and shifting the burden of financial risk directly onto the providers.
The Structural Mechanics of Financial Accountability
At the heart of this initiative lies a sophisticated financial framework that holds hospitals strictly accountable for the total cost of a patient’s care episode against a predetermined target price. This target price is not a static number but is calculated using historical data and regional benchmarks to ensure that the expectations remain realistic yet challenging for various types of facilities. If a hospital manages to keep the total cost of the ninety-day episode below the target while meeting specific quality metrics, it becomes eligible for an additional payment from Medicare, representing a share of the savings achieved. However, the model carries significant downside risk, as facilities that exceed their budgets may be required to repay the difference to the federal government. To mitigate the impact on specialized institutions, CMS has incorporated a robust risk adjustment methodology involving twenty-nine distinct adjusters, which accounts for patient complexity and socio-economic factors more accurately than any previous pilot program or voluntary model.
To provide a safety net for institutions serving vulnerable populations, the program includes a five percent stop-loss protection specifically for hospitals that manage high volumes of dual-eligible patients. This provision acknowledges that patients who qualify for both Medicare and Medicaid often present with more complex social needs and comorbidities that can naturally drive up recovery costs. By limiting the financial liability for these specific providers, the federal government aims to prevent a scenario where high-risk patients are avoided in favor of healthier individuals who are easier to manage within a budget. Furthermore, the mandatory nature of this model across the country ensures a level playing field, preventing hospitals from opting out of value-based care when the financial stakes become high. This creates a competitive environment where the primary differentiator is no longer just the volume of surgeries performed but the efficiency and effectiveness of the long-term recovery process managed by the surgical team and their partners.
Navigating Shifts in the Post-Acute Care Continuum
Skilled nursing facilities and inpatient rehabilitation centers are facing a period of significant transition as the new payment model incentivizes hospitals to steer patients toward home-based recovery. Data observed between 2026 and 2028 indicates that the original pilot programs for joint replacements achieved substantial savings primarily by reducing the utilization of high-cost institutional post-acute care. When hospitals are financially responsible for the total cost of an episode, they naturally favor outpatient rehabilitation or home health services, which are often preferred by patients and significantly less expensive for the system. This trend is further supported by the federal decision to waive certain regulatory barriers, such as the mandatory three-day hospital stay requirement previously necessary for Medicare to cover skilled nursing facility services. These waivers provide surgeons with the clinical flexibility to discharge patients directly to their preferred recovery environment without being hindered by outdated administrative hurdles.
Despite the shift toward home-based care, skilled nursing facilities remain a critical component of the care continuum for patients with severe comorbidities or those lacking adequate support systems at home. For these operators, the challenge lies in demonstrating exceptional value and clinical outcomes to their hospital partners to remain a preferred destination in a cost-conscious market. Many facilities are responding by investing in specialized orthopedic rehabilitation programs and advanced telemetry tools that allow for better communication with the referring hospital’s care coordinators. This integration is essential because any complication or readmission within the ninety-day window directly impacts the hospital’s financial performance under the new model. Consequently, the relationship between hospitals and post-acute providers is evolving from a simple referral handshake into a deep, data-driven partnership where both parties are aligned on the goal of minimizing recovery time while maximizing functional independence for the patient.
Implementing Strategic Solutions for Future Success
As the healthcare industry prepares for the full implementation of this model, healthcare administrators must prioritize the adoption of integrated data platforms that provide real-time visibility into the patient’s progress after they leave the hospital. Successful organizations will likely find that investing in dedicated navigators or transitional care managers pays for itself by preventing avoidable emergency department visits and ensuring adherence to physical therapy protocols. These professionals act as the connective tissue between the surgeon, the primary care physician, and the post-acute team, identifying potential red flags before they escalate into costly complications. Moreover, leveraging predictive analytics can help surgical teams identify which patients are at the highest risk for readmission, allowing for a more personalized and intensive follow-up strategy during the critical first thirty days after surgery. This proactive approach moved the needle during the experimental phases and will be the standard for the upcoming mandatory cycle.
Looking ahead, the long-term viability of orthopedic programs will depend on their ability to treat the surgical episode as a continuous narrative rather than a series of disconnected events. Hospitals should begin auditing their existing partnerships with home health agencies and skilled nursing facilities to ensure that every participant in the care chain is committed to the same clinical and financial objectives. Organizations that wait until the mandatory deadline to refine their processes will likely struggle with the financial penalties associated with exceeding target prices. Instead, facilities should use the current period to pilot internal cost-tracking mechanisms and establish clear communication channels with their community partners. By focusing on the total patient experience and utilizing the flexibilities provided by the program waivers, providers can transform a regulatory mandate into a strategic advantage that improves patient satisfaction and stabilizes institutional revenue for the coming years.