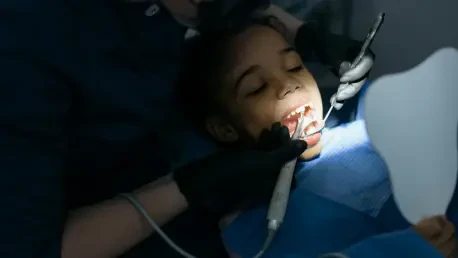
The sight of a five-year-old child suffering from avoidable dental pain serves as a stark reminder that public health successes are often distributed unevenly across different social strata. According to the latest findings from the NHS Wales Dental Epidemiology Programme, which examined over 8,500 children in their first year of school, there is a clear and quantifiable improvement in oral health across the nation. Specifically, the data indicates that the prevalence of tooth decay in this age group fell to 27 percent during the recent assessment period, marking a notable decrease from the 32.4 percent recorded in previous years. This downward trajectory reflects a sustained effort that began nearly two decades ago, effectively reducing the number of children with dental issues in an average classroom from fourteen to just eight. While these statistics highlight a broad victory for preventative medicine, they also mask the deeper complexities of a healthcare system struggling to ensure that every child, regardless of their background, benefits from these advancements equally.
Evolution of Pediatric Oral Health Outcomes
Shifting Trends in Disease Prevalence
The consistent decline in dental caries among young children is largely attributed to the successful integration of school-based health initiatives and community-wide education efforts. Programs like “Designed to Smile” have played a pivotal role by bringing fluoride varnish applications and supervised toothbrushing directly into the classroom environment. By normalizing oral hygiene as a daily educational activity, health officials have managed to reach thousands of children who might otherwise lack consistent access to dental care at home. This systematic approach has significantly lowered the national average of decay, proving that targeted interventions can yield measurable results when supported by long-term funding and political will. However, the data suggests that while the number of children entering school with healthy teeth is increasing, those who do suffer from decay are often dealing with more aggressive forms of the disease. This reality necessitates a shift in focus from broad-based prevention to more intensive, specialized support for the remaining demographic that remains high-risk.
The Impact of Dental Distress on Daily Life
Beyond the statistical prevalence of decay, the severity of dental disease continues to place a heavy burden on the well-being of young children and their families. For those who are diagnosed with caries, the impact is often profound, with an average of 3.5 teeth being affected per child, which indicates that the disease is frequently advanced by the time it is detected. This clinical severity manifests in the daily lives of families as persistent pain and functional limitations; nearly 25 percent of parents with children suffering from decay reported that their child experienced significant dental pain over the past year. Furthermore, the psychological and social ramifications are evident, as almost 39 percent of these parents noted a negative effect on their child’s overall quality of life, a figure that is more than double the rate observed in the general population. Such findings underscore that dental health is not merely a cosmetic or isolated issue but a fundamental component of childhood development that influences sleep, nutrition, and even the ability to concentrate in school.
Socioeconomic Disparities and Preventative Strategies
The Persistent Divide in Community Health
Despite the overall reduction in tooth decay across the country, a troubling stagnation in health equality has become the primary concern for policymakers and medical professionals. The gap between children living in the most affluent areas and those in the most deprived communities has remained virtually unchanged for over a decade, indicating that general improvements have not bridged the socioeconomic divide. Children from lower-income backgrounds are still disproportionately likely to experience severe dental issues, often lacking the resources or local infrastructure needed to maintain optimal oral health. This persistent inequality suggests that a “one-size-fits-all” approach to public health may have reached its limit in terms of efficacy. To address this disparity, future strategies must look beyond school-based programs and delve into the root causes of health inequality, such as the availability of affordable fresh food and the proximity of dental practices to marginalized neighborhoods. Ensuring that the most vulnerable populations receive enhanced support is the only way to achieve true parity.
Future Directions for Equitable Care
The path forward required a multifaceted commitment to dietary reform and the reinforcement of daily hygiene habits within the home environment. Public health experts emphasized that reducing sugar consumption in early childhood remained the most effective way to prevent the onset of decay before children even reached school age. Furthermore, the consistent use of age-appropriate fluoride toothpaste twice a day was identified as a non-negotiable standard for maintaining dental integrity. Regular attendance at professional dental appointments also served as a critical safeguard, allowing for early intervention and the application of preventative treatments like sealants. To sustain the progress observed in recent years, the government prioritized targeted investments in the most deprived regions, ensuring that financial barriers did not prevent families from accessing necessary care. By focusing on these localized solutions and fostering a culture of oral health awareness, the healthcare system aimed to eliminate the existing disparities. These actions collectively ensured that the gains made in pediatric dentistry were shared by all children.