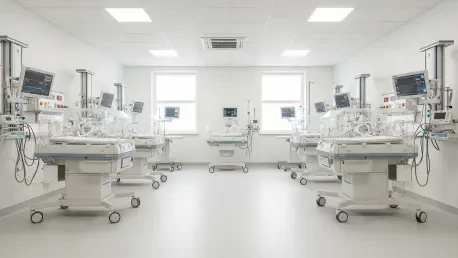
The transition to the state-of-the-art Ksyen Regional Hospital was intended to mark a new era of medical excellence for the northern region, yet the gleaming facility remains a quiet monument to the nationwide shortage of specialized clinicians. While the physical infrastructure exists to provide life-saving care to the most vulnerable patients, the inability to secure qualified staff has stalled the activation of the highly anticipated Neonatal Intensive Care Unit. This specialized ward represents more than just additional beds; it is a critical link in the regional healthcare chain that aims to keep families together during their most trying moments. However, the complexity of neonatal care requires a specific subset of nursing expertise that is currently in high demand and low supply across the country. As administrators navigate these hurdles, the delay highlights the growing tension between modern facility design and the human capital required to breathe life into clinical spaces.
The Crisis of Specialized Healthcare Personnel
Barriers to Twenty-Four-Seven Specialized Coverage
Running a modern Neonatal Intensive Care Unit is not merely a matter of having the right incubators and monitors; it requires a deep bench of highly trained professionals capable of providing constant, vigilant care. Northern Health has identified a specific need for two specialized nursing roles that must be filled around the clock to ensure the safety of newborns. Because of the intensive nature of this work, maintaining a 24/7 presence for a single position requires the equivalent of four full-time employees to account for standard rotations, mandatory leave, and unexpected absences. This means the hospital needs a minimum of eight dedicated specialists just to open the doors of this single unit. The specialized training required for these roles is extensive, making the recruitment pool remarkably small in a competitive labor market. The facility currently possesses the high-tech infrastructure needed for advanced care, but the vacant shifts prevent the unit from meeting mandatory safety standards.
Broader Implications for Regional Medical Services
The staffing deficit at Ksyen Regional Hospital is not limited to the pediatric wing but echoes through various departments, impacting the overall breadth of care available to the community. For instance, the hospital’s 20-bed psychiatric unit, which serves a vital role in regional mental health, is currently forced to operate at only half its intended capacity due to a lack of qualified psychiatric nurses and support staff. Furthermore, plans to launch a 24/7 advanced trauma care service have been postponed, as the facility struggles to assemble the necessary team of emergency medicine specialists. Despite these significant systemic challenges, the hospital has managed to find success in other surgical areas, such as the successful initiation of full knee replacement surgeries. These procedures demonstrate that while the hospital is capable of high-level performance in elective and scheduled care, the unpredictability of intensive, around-the-clock emergency services remains hampered by the labor crisis.
Community Investment and the Path Toward Local Care
Financial Foundation and the Closer to Home Initiative
The drive to establish a local Neonatal Intensive Care Unit is fueled by a massive $14.5 million investment, a figure that reflects the deep commitment of both the government and the local community. A substantial portion of this funding, roughly $4.5 million, was raised through a dedicated community campaign led by the R.E.M. Lee Hospital Foundation, with the remainder sourced through regional property taxes. The primary objective of this project, titled “Closer to Home,” is to alleviate the immense emotional and financial burden placed on families who are currently forced to travel for specialized care. Under the current system, families often face the terrifying prospect of emergency medical flights to distant urban centers, separating parents from their support networks during medical crises. By establishing a local unit, the region seeks to provide a sense of stability and security, ensuring that vulnerable infants receive top-tier medical attention without the added trauma of long-distance relocation or the exorbitant costs of travel.
Strategic Recruitment and Future Operational Stability
To overcome the existing operational barriers, healthcare leaders shifted their focus toward long-term recruitment incentives and robust family support programs that address the realities of regional medical care. The R.E.M. Lee Hospital Foundation prioritized the development of a support system to assist parents with travel and lodging costs, ensuring that financial status never dictates a family’s proximity to their child. However, the ultimate success of the facility depended on a more aggressive approach to medical education and local training pipelines. Stakeholders recommended that regional authorities partner with educational institutions to create fast-track certification programs for specialized nursing, effectively growing the talent pool from within the community. Moving forward, the hospital must balance its reliance on external recruitment with sustainable internal development strategies. Future investments should be channeled into staff retention packages and housing solutions to make the region more attractive to specialized talent.